Insulin expires in two ways: the printed expiration date on unopened vials and 28 days after you first use a vial or pen. So, does insulin expire quickly once opened? Yes, using expired insulin reduces its effectiveness, which can lead to unpredictable blood sugar levels and complications. Proper storage, including refrigerating unopened insulin, keeping opened insulin at room temperature, and avoiding heat or freezing, is crucial for maintaining potency. Signs of bad insulin include clumping, cloudiness, unusual color, or floating particles. Never use expired insulin and dispose of it safely. Consistent timing of insulin doses, working closely with your healthcare provider, and monitoring blood sugar help ensure safe and effective diabetes management.
Does Insulin Expire? Understanding Shelf Life and Safety
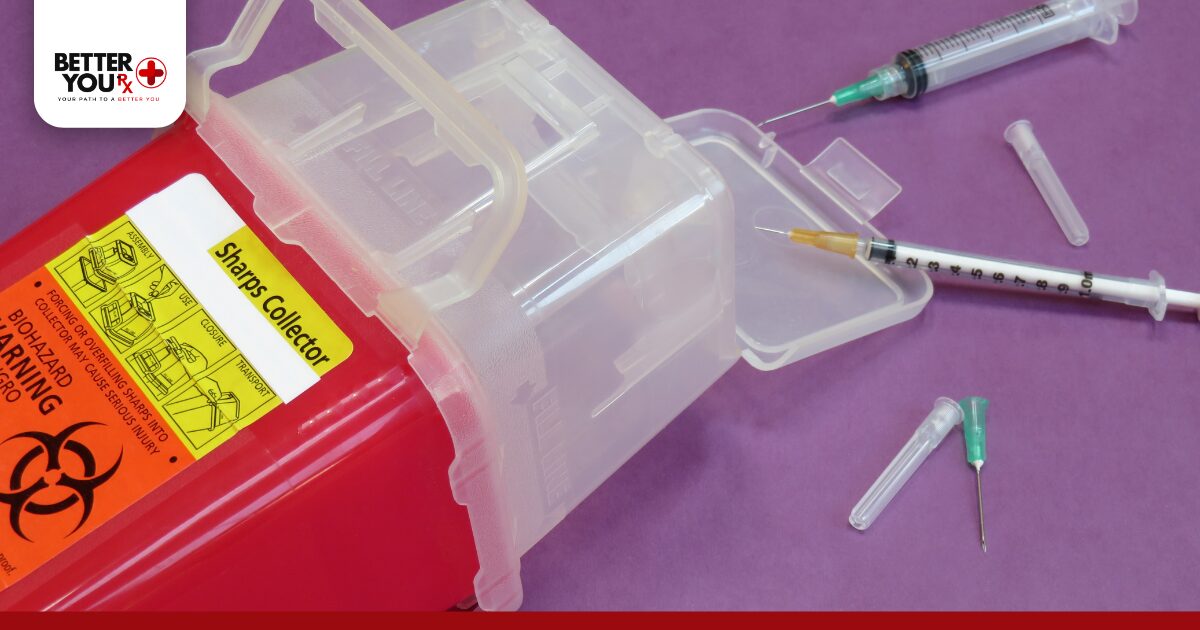
Yes, Insulin has two important expiration dates you need to track. The first is the manufacturer’s expiration date printed on the package, which applies to unopened insulin stored in the refrigerator. The second “expiration” happens once you start using it.
Here’s the breakdown:
- Unopened insulin: Lasts until the printed expiration date (usually 2-3 years from manufacture)
- Opened insulin: Good for 28 days at room temperature, regardless of the printed date
- Insulin pens: Same 28-day rule once you insert the first needle
The reason insulin expires is that it’s a protein-based hormone that breaks down over time, especially when exposed to heat, light, or temperature fluctuations. This breakdown makes it less effective at controlling your blood sugar levels.
Read more about proper insulin storage techniques and tips to extend your medication’s lifespan.
Is It Okay to Use Expired Insulin?
No, it’s not safe to use expired insulin. While it may not harm you immediately like spoiled food, expired insulin becomes unreliable, which can be dangerous for diabetes management.
When it has expired, its effectiveness becomes unpredictable. Even if you administer your usual dose, reduced potency may cause unexpected increases in blood glucose levels. This unpredictability can lead to:
- Sudden high blood sugar episodes
- Increased risk of diabetic complications
- Difficulty maintaining your regular diabetes routine
- Potential emergency situations
Some individuals may believe that using expired insulin is preferable to taking none, but this can lead to a false sense of safety. If you only have expired insulin available, consult your healthcare provider immediately for guidance instead of self-administering a potentially ineffective medication.
You can check out our insulin medications to ensure you always have fresh, effective insulin on hand.
Does Insulin Lose Its Effectiveness?
Yes, insulin gradually loses its effectiveness over time, and this process accelerates once the vial or pen is opened. The potency doesn’t disappear overnight – it’s more like a slow fade.
| Storage Condition | Effectiveness Timeline |
| Refrigerated, unopened | Maintains full potency until expiration date |
| Room temperature, opened | Begins losing potency after 28 days |
| Exposed to heat/sunlight | Rapid potency loss within hours |
| Frozen (accidentally) | Immediate and permanent potency loss |
The effectiveness loss isn’t linear either. In the first few weeks after opening, you might not notice much difference. But as you approach that 28-day mark, it becomes increasingly unreliable. Some doses might work fine, while others might leave you with higher blood sugar than expected.
Temperature plays a huge role in this process. If it is stored in a hot car, left in direct sunlight, or exposed to freezing temperatures, it can lose effectiveness much faster than the standard timeline suggests.
Buy affordable Humalog KwikPen online through Better You Rx to maintain a reliable supply of effective insulin.
What Happens If You Inject Bad Insulin?
Injecting bad or expired insulin typically does not cause immediate physical harm like an allergic reaction, but can create serious blood sugar management issues.
Immediate effects:
- Higher than expected blood glucose readings
- Increased thirst or hunger
- Increased urination
- Fatigue or sluggishness
Longer-term concerns:
- Difficulty maintaining target blood sugar ranges
- Increased risk of diabetic complications
- Potential for diabetic ketoacidosis in severe cases
- Disruption of established diabetes management routines
Bad insulin may not fail completely, sometimes working partially, making it difficult to recognize the medication as the problem. Patients may attribute poor control to other factors when the insulin itself is compromised.
If patients suspect they have been using bad insulin, they should check blood sugar more frequently and contact their healthcare provider to discuss temporary treatment plan adjustments.
What to Do With Old Insulin?
Insulin should never be thrown in regular trash or flushed down the toilet. Proper disposal is required to protect the environment and prevent accidental exposure.
Proper disposal steps:
- Remove needles and dispose of them in a sharps container
- Keep insulin in its original packaging when possible
- Use community medication disposal events
- Utilize special medical waste disposal sites where available
Patients should not keep expired insulin “just in case” to save money. The risk of unreliable blood sugar control outweighs potential savings. Instead, work with healthcare providers and insurance to ensure a steady supply of fresh insulin.
What Are the Symptoms of Bad Insulin?
Recognizing bad insulin isn’t always straightforward since the symptoms mimic general blood sugar management issues. However, there are some signs to watch for:
Physical signs in the insulin itself:
- Clumping or crystallization in clear insulin
- Cloudiness in rapid-acting insulin (which should be clear)
- Changes in color or consistency
- Floating particles or residue
- Unusual odor
Symptoms in your body:
- Consistently higher blood sugar readings despite normal routine
- Increased thirst and urination
- Unexplained fatigue
- Difficulty achieving target glucose levels
- Blood sugar spikes that don’t respond to your usual correction doses
Pattern recognition:
- Good control suddenly becomes erratic
- Need for higher insulin doses without lifestyle changes
- Morning blood sugars consistently higher than usual
If you notice any of these signs, don’t wait to see if things improve. Switch to a fresh vial or pen if you have one available, and monitor your blood sugar closely. Keep detailed records to share with your healthcare provider.
When Is the Best Time to Take Insulin for Type 2 Diabetes?
The timing of insulin administration depends on the type of insulin you’re using and your individual diabetes management plan. However, there are some general guidelines that work for most people with type 2 diabetes.
Long-acting insulin:
- Take at the same time every day (many prefer bedtime)
- Provides baseline insulin coverage for 24 hours
- Timing consistency is more important than the specific time chosen
Rapid-acting insulin:
- Take 15-20 minutes before meals
- Helps manage blood sugar spikes from food
- Timing should align with your eating schedule
Factors that affect timing:
- Your work schedule and meal times
- Exercise routine
- Sleep patterns
- Other medications you’re taking
The key is consistency. Your body responds best when insulin administration follows a predictable pattern. Work with your healthcare provider to establish a schedule that fits your lifestyle while maintaining good blood sugar control.
Remember, these are general guidelines – your specific insulin regimen should always be based on your healthcare provider’s recommendations and your individual needs.
Wrapping Up
Managing insulin expiration dates is a crucial part of diabetes care that many people overlook. The bottom line is simple: insulin does expire, and using expired insulin can put your health at risk through unpredictable blood sugar control.
Here’s what you need to remember: unopened insulin lasts until its printed expiration date when refrigerated, but once opened, you have just 28 days regardless of what the package says. Never ignore the warning signs of bad insulin like clumping, cloudiness, or consistently high blood sugar readings.
The key to successful diabetes management is consistency and reliability. This means using fresh, effective insulin and taking it at the same time each day based on your healthcare provider’s guidance. Don’t risk your health trying to stretch expired insulin – work with your insurance and healthcare team to maintain a steady supply of fresh medication.
By staying on top of expiration dates and recognizing the signs of compromised insulin, you’re taking an important step toward better diabetes management and overall health. When in doubt, always consult with your healthcare provider rather than guessing about insulin safety.
Frequently Asked Questions
What Not to Do When Injecting Insulin?
Avoid injecting insulin into the same exact spot repeatedly, as this can cause lumps under the skin. Don’t inject into areas that are bruised, scarred, or irritated. Also, never reuse needles, and always make sure your hands and injection site are clean.
Is 20 Units of Insulin a Lot?
Whether 20 units is a lot depends on the individual, their condition, and their doctor’s instructions. For some people, it may be a normal dose, while for others it may be too much or too little. Always follow the guidance of your healthcare provider.
How Much Insulin Should I Take If My Blood Sugar Is 250?
Insulin needs vary from person to person. There is no one-size-fits-all dose for high blood sugar levels like 250. The correct adjustment should be based on your doctor’s instructions, your insulin sensitivity, and your prescribed correction factor.
How Do I Know If My Insulin Is Good?
Check the expiration date and look at the insulin itself. It should be clear (if it’s rapid-acting or long-acting clear insulin) or evenly cloudy (for NPH). If you see clumps, discoloration, or crystals, do not use it.
When Should You Throw Away Insulin?
Insulin should be thrown away once it expires or 28–56 days after opening, depending on the type and storage conditions. Always check the manufacturer’s instructions for the exact time frame.
Can Too Much Insulin Raise Blood Sugar?
No, too much insulin does not raise blood sugar. Instead, it lowers blood sugar, sometimes to dangerous levels. However, frequent low blood sugar can trigger your body to release stress hormones, which may later cause rebound high blood sugar.
Is Expired Insulin Still Effective?
Expired insulin is less effective and may not control blood sugar properly. Using it could lead to dangerously high blood sugar levels. It’s always safest to use insulin that is within its expiration date.