Weight-based insulin dosing represents a fundamental approach to diabetes management that helps healthcare providers determine appropriate insulin doses based on a patient’s body weight. This comprehensive guide explores the essential principles of calculating weight-based insulin doses, understanding different insulin types, and implementing safe dosing strategies for effective blood sugar control.
The weight-based dosing method provides a starting point for insulin therapy by establishing baseline requirements typically ranging from 0.4 to 1.0 units per kilogram of body weight daily. This approach considers individual factors such as insulin sensitivity, activity levels, and disease progression while offering healthcare providers a systematic framework for initiating and adjusting insulin therapy.
Understanding Weight-Based Insulin Calculations
Weight-based insulin dosing serves as the foundation for establishing appropriate insulin therapy in diabetes management. The calculation process begins with determining total daily insulin requirements based on body weight, typically measured in kilograms. Healthcare providers use established formulas that account for different patient populations and insulin sensitivity levels.
The basic calculation starts with multiplying body weight in kilograms by a predetermined factor ranging from 0.4 to 1.0 units per kilogram. Newly diagnosed patients with type 1 diabetes often begin with lower doses around 0.4-0.6 units per kilogram, while patients with insulin resistance or type 2 diabetes may require higher doses approaching 0.8-1.0 units per kilogram or more.
Patient factors significantly influence these calculations including age, physical activity level, eating patterns, and concurrent medications. Younger patients typically demonstrate higher insulin sensitivity requiring lower doses per kilogram, while older adults or those with additional health conditions may need adjusted calculations. The presence of other medications, particularly corticosteroids or certain psychiatric medications, can increase insulin requirements substantially.
Looking to optimize your diabetes management with reliable insulin options? Consider Humalog Junior KwikPen for precise pediatric dosing needs.
How to Calculate Weight-Based Insulin Dosing
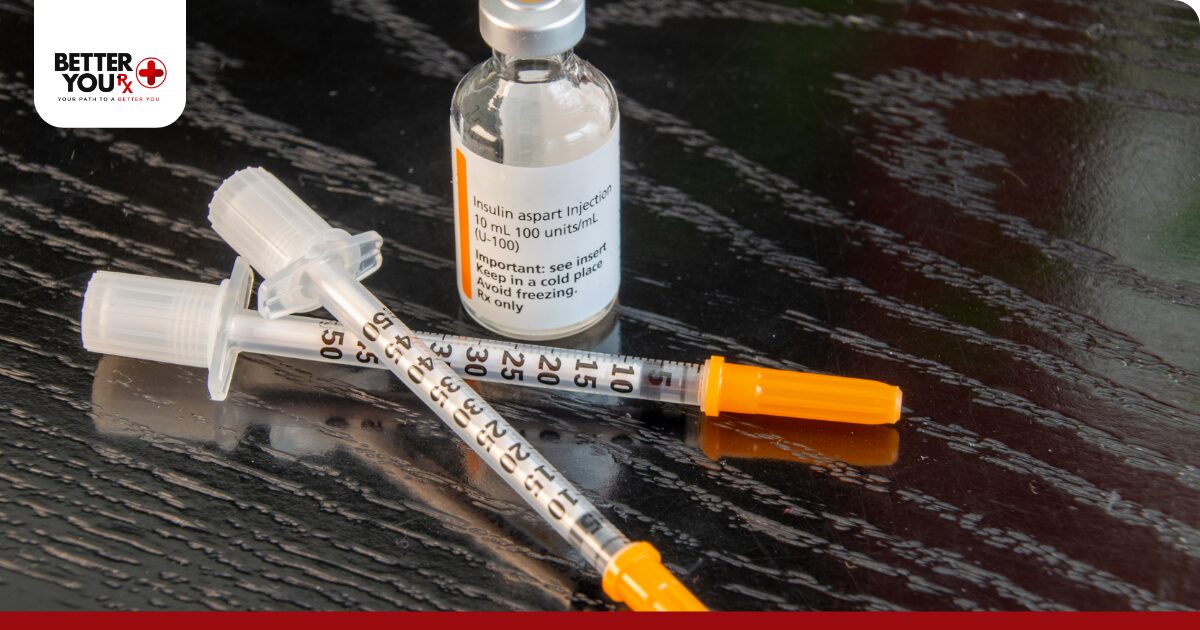
Calculating weight-based insulin dosing involves several systematic steps that healthcare providers follow to establish safe and effective insulin regimens. The process requires accurate body weight measurements, understanding of insulin types, and consideration of individual patient factors.
Step 1 – Determine Total Daily Insulin Dose (TDID) Begin by calculating the total daily insulin dose using the formula: TDID = Body weight (kg) × Units per kg factor. For most patients, start with 0.5 units per kilogram as a baseline, adjusting based on individual circumstances.
Step 2 – Distribute Between Basal and Bolus Insulin Divide the total daily dose between basal (background) insulin and bolus (mealtime) insulin. Typically, 40-50% of the total dose serves as basal insulin, while the remaining 50-60% covers bolus needs distributed across meals.
Step 3 – Calculate Individual Meal Bolus Doses Distribute bolus insulin across meals based on carbohydrate content and individual insulin-to-carbohydrate ratios. Start with dividing bolus insulin equally across three meals, then adjust based on actual carbohydrate intake and blood glucose responses.
Step 4 – Apply Correction Factors Establish correction factors for high blood glucose levels, typically starting with 1 unit of rapid-acting insulin for every 50 mg/dL above target glucose levels. Adjust this sensitivity factor based on individual response patterns and total daily insulin requirements.
The calculation process requires ongoing monitoring and adjustment based on blood glucose patterns, lifestyle changes, and patient response to initial dosing recommendations.
Types of Weight-Based Insulin Dosing Regimens
Different insulin regimens utilize weight-based calculations while addressing varying patient needs and diabetes management goals. Understanding these regimens helps healthcare providers select appropriate approaches for individual patients.
Basal-Bolus Regimens Basal-bolus regimens provide the most physiologic approach to insulin replacement therapy. Long-acting insulin such as Glargine or Detemir covers basal needs, while rapid-acting insulin like Lispro or Aspart addresses mealtime requirements. Weight-based calculations determine both components with typical distributions of 40-50% basal and 50-60% bolus insulin.
Mixed Insulin Regimens Pre-mixed insulin combinations like 70/30 or 75/25 formulations offer convenience for patients requiring simplified regimens. Weight-based dosing for mixed insulins typically starts with 0.6-0.8 units per kilogram daily, divided between morning and evening doses based on individual meal patterns and glucose responses.
Sliding Scale Approaches While less preferred for routine management, sliding scale insulin protocols use weight-based corrections for hospitalized patients or temporary situations. These protocols establish correction doses based on current blood glucose levels and total daily insulin requirements calculated from patient weight.
Continuous Insulin Infusion Insulin pump therapy utilizes sophisticated weight-based calculations for programming basal rates and bolus doses. Initial pump settings derive from total daily injection requirements, with basal rates typically programmed as 40-50% of total daily needs distributed across 24-hour periods.
Factors Affecting Weight-Based Insulin Requirements
Multiple factors influence individual insulin requirements beyond simple weight-based calculations. Understanding these variables helps healthcare providers make appropriate adjustments and set realistic expectations for diabetes management outcomes.
Insulin Sensitivity Variations Individual insulin sensitivity varies significantly based on factors including genetics, physical fitness, body composition, and hormonal status. Athletes or physically active individuals often demonstrate higher insulin sensitivity requiring lower doses per kilogram, while sedentary patients may need higher doses to achieve similar glucose control.
Age-Related Considerations Age significantly impacts insulin requirements with children and adolescents often requiring higher doses per kilogram due to growth hormone effects and pubertal changes. Elderly patients may need lower starting doses due to decreased kidney function, reduced caloric intake, or increased risk of hypoglycemia.
Honeymoon Period Effects Newly diagnosed type 1 diabetes patients may experience a honeymoon period where remaining beta cell function reduces insulin requirements. During this phase, weight-based calculations may overestimate needs, requiring careful monitoring and dose reductions to prevent hypoglycemia.
Concurrent Medical Conditions Various medical conditions affect insulin requirements including kidney disease, liver dysfunction, thyroid disorders, and infections. Kidney disease may reduce insulin clearance requiring dose adjustments, while hyperthyroidism can increase insulin needs substantially.
Medication Interactions Certain medications significantly impact insulin requirements including corticosteroids (increase needs), beta-blockers (may mask hypoglycemia symptoms), and some psychiatric medications (increase insulin resistance). Weight-based calculations must account for these interactions.
Safety Considerations and Monitoring
Safe implementation of weight-based insulin dosing requires comprehensive monitoring protocols and awareness of potential complications. Healthcare providers must establish clear guidelines for dose adjustments and patient education regarding hypoglycemia recognition and treatment.
Blood Glucose Monitoring Requirements Patients beginning weight-based insulin regimens require frequent blood glucose monitoring to assess dose appropriateness and identify patterns requiring adjustment. Initial monitoring typically includes pre-meal and bedtime glucose checks, with additional testing during illness or routine changes.
Hypoglycemia Prevention Weight-based dosing calculations provide starting points that require individualization to prevent hypoglycemia. Healthcare providers must educate patients about hypoglycemia symptoms, treatment protocols, and situations requiring immediate medical attention. Glucagon prescriptions become essential safety measures for patients using insulin.
Dose Adjustment Protocols Systematic dose adjustment protocols help healthcare providers make safe modifications to weight-based insulin regimens. Typical adjustment increments range from 10-20% of current doses, with changes made every 3-5 days based on glucose pattern analysis rather than isolated high or low readings.
Special Population Considerations Pregnant women, elderly patients, and those with kidney or liver disease require modified approaches to weight-based insulin dosing. These populations often need more conservative starting doses and more frequent monitoring to ensure safety while achieving glucose targets.
Insulin Types and Weight-Based Applications
| Insulin Type | Onset | Peak | Duration | Weight-Based Dosing Application |
| Rapid-Acting (Lispro, Aspart) | 15-30 min | 1-2 hours | 3-5 hours | Bolus dosing: 50-60% of TDID |
| Short-Acting (Regular) | 30-60 min | 2-4 hours | 6-8 hours | Mealtime coverage: 0.1-0.3 u/kg per meal |
| Intermediate-Acting (NPH) | 1-3 hours | 6-8 hours | 12-16 hours | Basal coverage: 40-50% of TDID |
| Long-Acting (Glargine, Detemir) | 1-4 hours | Minimal peak | 20-24 hours | Basal dosing: 0.2-0.5 u/kg daily |
| Pre-Mixed (70/30, 75/25) | 15-30 min | 2-8 hours | 16-20 hours | Twice daily: 0.3-0.4 u/kg per dose |
Different insulin types require specific considerations when applying weight-based dosing calculations. Rapid-acting insulins like Lispro and Aspart work quickly to cover mealtime glucose rises, while long-acting formulations provide steady background insulin coverage throughout the day.
Understanding pharmacokinetic profiles helps healthcare providers optimize timing and dosing for individual patient needs. The table above illustrates how different insulin types fit into weight-based regimens and typical dosing ranges for each category.
Special Dosing Situations and Adjustments
Certain situations require modifications to standard weight-based insulin dosing approaches. These circumstances demand careful consideration and often more intensive monitoring to ensure patient safety and optimal glucose control.
Sick Day Management Illness typically increases insulin requirements due to stress hormones and reduced food intake patterns. Patients may need 10-20% increases in total daily insulin doses during illness, with emphasis on maintaining basal insulin even when unable to eat normally. Blood glucose monitoring becomes more frequent during sick days.
Exercise and Physical Activity Regular exercise affects insulin sensitivity and may require dose adjustments to prevent hypoglycemia. Patients engaging in prolonged or intense physical activity often need 25-50% reductions in rapid-acting insulin doses for meals preceding exercise. Long-term exercise programs may reduce overall insulin requirements.
Travel and Schedule Changes Time zone changes and altered meal schedules require insulin timing adjustments while maintaining appropriate total daily doses. Patients crossing multiple time zones may need temporary intermediate adjustments before resuming normal schedules in new locations.
Pregnancy Considerations Pregnancy significantly alters insulin requirements with needs typically increasing throughout gestation. First trimester may see decreased requirements, while second and third trimesters often require substantial dose increases. Weight-based calculations must account for both pre-pregnancy weight and gestational changes.
Ready to start your Insulin Dosing Weight-Based journey? Explore Humulin N KwikPen for reliable intermediate-acting insulin coverage that fits seamlessly into your diabetes management plan.
Advanced Dosing Strategies
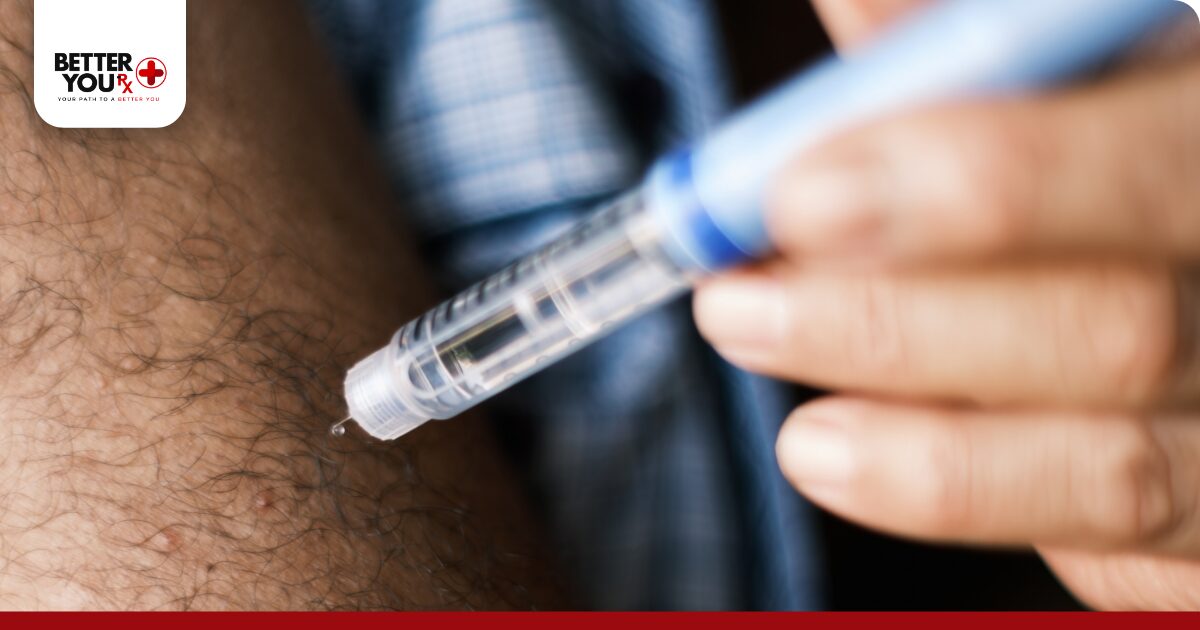
Advanced weight-based insulin dosing strategies incorporate sophisticated approaches that address complex diabetes management situations. These strategies often combine multiple calculation methods and require experienced healthcare provider guidance.
Carbohydrate-to-Insulin Ratios Individual carbohydrate-to-insulin ratios determine how much rapid-acting insulin patients need for specific amounts of dietary carbohydrates. Starting ratios often derive from weight-based calculations using the 450 rule (450 divided by total daily insulin dose) or 500 rule for more insulin-sensitive patients.
Correction Factor Calculations Correction factors help patients adjust insulin doses for elevated blood glucose levels. The 1800 rule (1800 divided by total daily insulin dose) provides starting correction factors, indicating how much blood glucose decreases per unit of rapid-acting insulin.
Pattern Management Advanced dosing involves analyzing blood glucose patterns over multiple days to identify consistent trends requiring systematic dose adjustments. Dawn phenomenon, post-meal spikes, and overnight lows each require specific modification strategies based on pattern timing and magnitude.
Technology Integration Modern diabetes technology including continuous glucose monitors and insulin pumps utilize weight-based calculations as starting points for automated dosing adjustments. These systems learn individual response patterns and modify doses based on real-time glucose data and historical patterns.
Need rapid-acting insulin for precise mealtime control? Discover Admelog Vial – the trusted choice for effective insulin dosing weight-based management that adapts to your lifestyle.
Key Takeaways for Successful Weight-Based Insulin Management
Successful weight-based insulin dosing requires systematic approaches combining accurate calculations with individualized adjustments based on patient response patterns. Healthcare providers must balance standard dosing formulas with patient-specific factors including lifestyle, concurrent medications, and individual insulin sensitivity variations.
Regular monitoring and systematic dose adjustments ensure optimal glucose control while minimizing hypoglycemia risks. Patients require comprehensive education about their insulin regimens including proper timing, dose calculations, and emergency management procedures for both high and low blood glucose situations.
The integration of modern diabetes technology with traditional weight-based calculations offers enhanced precision and safety for insulin dose management. Continuous glucose monitoring and insulin delivery systems provide real-time feedback for optimizing doses while maintaining the fundamental principles of weight-based dosing as starting points.
Long-term success with weight-based insulin dosing depends on consistent healthcare provider collaboration, patient education, and willingness to make appropriate adjustments based on changing circumstances and individual response patterns.
Frequently Asked Questions
What Is the 70 30 Rule Insulin?
The 70/30 rule refers to pre-mixed insulin containing 70% intermediate-acting insulin (NPH) and 30% short-acting regular insulin. Weight-based dosing typically starts with 0.6-0.8 units per kilogram daily, divided between morning (60-70%) and evening (30-40%) doses.
How Much Insulin per Kg Body Weight?
Type 1 diabetes patients typically need 0.4-1.0 units per kilogram daily. Newly diagnosed patients start at 0.4-0.6 u/kg, while established patients require 0.6-1.0 u/kg. Type 2 diabetes patients may need 0.8-2.0 units per kilogram daily due to insulin resistance.
What Is the 2/3 1/3 Rule for Insulin?
The 2/3 1/3 rule distributes total daily insulin dose with two-thirds given in the morning and one-third in the evening. This accounts for higher daytime insulin needs when cortisol levels and food intake are greater.
What Is the 30 60 90 Rule for Insulin?
The 30 60 90 rule refers to blood glucose monitoring times after insulin injection. Check at 30 minutes for immediate effects, 60 minutes for peak action, and 90 minutes for overall effectiveness. This helps determine if ratios need adjustment.
How Does Weight Affect Insulin Needs?
Higher body weight often increases insulin resistance, requiring more units per kilogram. Muscle mass increases insulin sensitivity while fat tissue decreases it. Weight changes typically require 10% dose adjustments for every 10% weight change.
How Much Insulin Should I Take if My Sugar Is 300?
Correction doses depend on individual factors. A typical correction might be 1 unit per 50 mg/dL above target. For 300 mg/dL with a 120 mg/dL target: (300-120)/50 = 4 units. Healthcare providers must determine individual correction factors.
What Is the 3 Hour Rule for Diabetes?
Rapid-acting insulin remains active for approximately 3 hours. Avoid giving additional doses within 3 hours of the previous injection unless directed by healthcare providers to prevent dangerous insulin stacking and hypoglycemia.