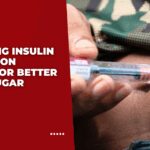
Places to inject insulin include the abdomen, thighs, upper arms, and buttocks, each offering different absorption rates that affect blood sugar control. The abdomen provides the fastest and most consistent absorption, making it the preferred site for mealtime insulin doses. Rotating injection sites within each area prevents lipodystrophy, a condition causing lumpy or indented skin that impairs insulin absorption. Proper injection technique involves selecting fatty tissue areas, avoiding muscles, scars, and bruised areas while maintaining at least one inch distance between injection points. Temperature, exercise, and massage can alter absorption rates at injection sites, requiring adjustments in timing and location selection based on daily activities.
Why Injection Site Selection Matters for Blood Sugar Control
Selecting appropriate places to inject insulin directly impacts how quickly and effectively the medication enters your bloodstream. Different body areas have varying blood flow rates and fat distribution, creating significant differences in absorption timing. The abdomen typically absorbs insulin within 15-30 minutes, while thigh injections may take 45-60 minutes to reach peak absorption.
Consistent site selection helps maintain predictable blood sugar patterns. Using the same general area for specific insulin types – such as always injecting rapid-acting insulin in the abdomen before meals – creates reliable timing patterns. This consistency allows for better dose calculations and reduces unexpected blood sugar variations.
Poor injection site management leads to several complications:
- Lipodystrophy development from repeated use of the same spot
- Unpredictable absorption causing blood sugar swings
- Increased pain and bruising from overused areas
- Reduced insulin effectiveness requiring higher doses
- Skin infections from inadequate site rotation
- Scar tissue formation blocking proper absorption
Blood flow variations throughout the day affect absorption at different places to inject insulin. Morning injections may absorb differently than evening ones due to circadian rhythm changes. Physical activity increases blood flow to exercised muscles, accelerating insulin absorption from nearby injection sites. Hot showers or baths similarly speed absorption through increased circulation.
Individual anatomy influences optimal site selection. People with more subcutaneous fat have greater flexibility in choosing injection locations. Those with less body fat must carefully identify appropriate areas with sufficient tissue depth. Body composition changes from weight loss or gain require reassessment of suitable injection sites.
Understanding the Four Main Places to Inject Insulin

The abdomen remains the most popular injection site due to its large surface area and consistent absorption rates. This area spans from below the ribs to above the hip bones, excluding a two-inch circle around the navel. Abdominal fat typically maintains steady thickness, providing reliable absorption regardless of weight fluctuations.
Abdomen – The Primary Injection Zone
Abdominal injections offer several advantages for daily insulin management. The area provides easy access for self-injection and visual confirmation of proper technique. Absorption remains relatively unaffected by physical activity compared to limb injection sites. The large surface area accommodates extensive rotation patterns, reducing tissue damage risk.
Divide your abdomen into quadrants for systematic rotation. Start injections in the upper right quadrant, moving systematically through each section before returning to the starting area. Maintain at least one finger-width spacing between injection points. This methodical approach ensures adequate healing time between site uses.
Thigh Injections – Alternative Sites
Thigh surfaces provide substantial injection area, particularly beneficial for people requiring multiple daily doses. The outer thigh area, from four inches below the hip to four inches above the knee, offers the best absorption consistency. Avoid inner thigh areas where skin folds and movement may affect needle placement.
Thigh absorption rates vary more than abdominal sites due to muscle proximity and activity levels. Walking, running, or cycling significantly increases absorption speed from recent thigh injections. Consider this acceleration when planning injection timing around exercise schedules.
Upper Arm Considerations
The upper arm’s outer surface provides convenient places to inject insulin, though self-injection proves challenging without assistance. The injectable area extends from three inches below the shoulder to three inches above the elbow on the arm’s outer aspect. Limited fat tissue in many individuals restricts this site’s usefulness.
Partner assistance often becomes necessary for proper upper arm injections. The awkward angle required for self-injection increases risk of intramuscular injection or improper needle insertion. Reserve this site for situations when other areas need rest or when someone can assist with injection.
Buttocks as Injection Sites
The upper outer buttocks offer excellent absorption for longer-acting insulins. This area typically contains substantial fat tissue, reducing injection discomfort. The site works particularly well for children who may resist visible injection locations. However, self-injection difficulty limits adult use of this area.
Proper Rotation Techniques for Healthy Injection Sites
Systematic rotation prevents the complications associated with repeatedly using the same places to inject insulin. Create a rotation schedule that allows each site at least one week of recovery before reuse. Document injection locations using a body map or smartphone app to track patterns and identify overused areas.
Establish zones within each injection area for organized rotation. The abdomen can accommodate 20-30 different injection points when properly mapped. Number or letter each zone mentally, progressing through them sequentially. This structured approach eliminates guesswork and ensures even site usage.
Creating Your Personal Rotation Map
Design a personalized rotation system based on your injection frequency and preferred sites. Weekly planners work well for visualizing rotation patterns. Assign specific areas to different days or insulin types. Morning long-acting doses might use right abdomen sections, while mealtime rapid-acting doses rotate through left abdomen areas.
| Day | Morning Site | Lunch Site | Dinner Site | Bedtime Site |
| Monday | Right upper abdomen | Left upper abdomen | Right thigh | Right buttock |
| Tuesday | Right lower abdomen | Left lower abdomen | Left thigh | Left buttock |
| Wednesday | Left upper abdomen | Right upper abdomen | Right arm | Right thigh |
| Thursday | Left lower abdomen | Right lower abdomen | Left arm | Left thigh |
| Friday | Right thigh | Left thigh | Right upper abdomen | Right buttock |
| Saturday | Left thigh | Right thigh | Left upper abdomen | Left buttock |
| Sunday | Right arm | Left arm | Lower abdomen | Alternate site |
Monitor each injection site for signs of overuse. Red marks persisting over 24 hours indicate inadequate healing time. Hard lumps or indentations suggest lipodystrophy development requiring immediate site abandonment. Persistent pain or tenderness warns of potential tissue damage.
Looking for reliable diabetes medications at competitive prices? Purchase authentic Trulicity from Canadian pharmacy partner through Better You Rx and save substantially on your prescription costs.
Factors Affecting Insulin Absorption at Different Sites
Temperature dramatically influences absorption rates at all places to inject insulin. Heat dilates blood vessels, accelerating insulin uptake by 50% or more. Cold constricts vessels, potentially doubling absorption time. Room temperature insulin absorbs most predictably, so remove refrigerated insulin 15-30 minutes before injection.
Exercise creates site-specific absorption changes lasting several hours post-activity. Leg exercises accelerate thigh injection absorption, while arm workouts affect upper arm sites similarly. Abdominal exercises have minimal impact on belly injection sites due to limited muscle involvement. Plan injection locations based on anticipated physical activities.
Body Composition and Site Selection
Individual fat distribution patterns determine optimal places to inject insulin for each person. Measure pinchable skin thickness at potential sites – adequate subcutaneous fat should create at least a half-inch fold. Insufficient fat tissue increases intramuscular injection risk, causing rapid, unpredictable absorption.
Weight changes require injection site reassessment. Weight loss may eliminate previously suitable areas, while weight gain opens new injection possibilities. Pregnancy particularly affects abdominal injection suitability as skin stretches and baby growth limits accessible areas.
Injection Depth and Angle Considerations
Needle length must match injection site characteristics to ensure subcutaneous delivery. Standard 4-6mm needles work for most adults at 90-degree angles. Thin individuals or children may require 45-degree angles or shorter needles to avoid muscle penetration. Longer 8-12mm needles necessitate pinching skin to create adequate fat layer depth.
The injection angle affects absorption consistency across different places to inject insulin. Perpendicular insertion typically provides most reliable delivery into subcutaneous tissue. Angled injections risk shallow placement in skin layers or deep penetration into muscle. Practice maintaining consistent angles regardless of injection location.
Common Injection Site Problems and Solutions
Lipodystrophy remains the most frequent complication from poor rotation of places to inject insulin. This condition manifests as either lipohypertrophy (fatty lumps) or lipoatrophy (indented areas). Both forms alter insulin absorption unpredictably, complicating blood sugar management. Complete avoidance of affected areas for 2-3 months often allows tissue recovery.
Bruising occurs from needle contact with capillaries during injection. While generally harmless, extensive bruising may indicate technique issues or overuse of specific sites. Apply gentle pressure without rubbing after injection to minimize bruising. Persistent bruising warrants technique review with healthcare providers.
Preventing and Managing Lipodystrophy
Early lipodystrophy detection enables successful treatment through site rest. Run your hands over injection areas weekly, feeling for unusual textures or contours. Visual inspection in good lighting reveals subtle skin changes before they become problematic. Photography helps track changes over time.
Recovery strategies for lipodystrophy include:
- Complete site abandonment for minimum three months
- Gentle massage of affected areas between injections
- Warm compress application to improve circulation
- Documentation of affected areas to prevent accidental use
- Dose adjustments when switching from affected to healthy sites
- Regular monitoring for improvement or worsening
Addressing Injection Pain and Discomfort
Injection discomfort often stems from poor technique rather than the places to inject insulin themselves. Room temperature insulin causes less pain than cold. Relaxed muscles accept injections more comfortably than tense ones. Quick, decisive insertion proves less painful than slow, hesitant movements.
Numbing techniques reduce injection discomfort for sensitive individuals. Ice application for 30-60 seconds before injection temporarily numbs the area. Commercial numbing creams provide longer-lasting relief but require advance application. Distraction techniques like deep breathing or counting help manage injection anxiety.
Need affordable alternatives for diabetes management? Buy cheap Victoza online from Canada and access quality medications at reduced prices.
Special Considerations for Different Insulin Types
Long-acting basal insulins like Lantus perform consistently across all standard places to inject insulin. These formulations’ extended release profiles minimize absorption rate variations between sites. However, maintaining site consistency improves predictability of overnight glucose control patterns.
Rapid-acting mealtime insulins benefit from faster-absorbing injection sites. The abdomen typically provides quickest absorption for pre-meal doses. Slower-absorbing sites like thighs work better for meals with extended digestion times, such as high-fat or high-protein foods.
Mixing Insulins and Site Selection
When combining insulin types in single injections, choose places to inject insulin based on the dominant insulin’s characteristics. NPH-regular combinations follow intermediate-acting absorption patterns. Site selection should prioritize consistency over absorption speed for mixed doses.
Pre-mixed insulin formulations require particularly careful site rotation. These products’ fixed ratios cannot accommodate site-specific absorption variations through dose adjustments. Establish dedicated rotation patterns for pre-mixed insulins to maintain stable blood sugar control.
Insulin Pump Sites
Insulin pump users face unique challenges selecting infusion sites. Continuous insulin delivery accelerates tissue changes at injection locations. Pump sites require rotation every 2-3 days, demanding larger rotation areas than injection users. The abdomen typically provides best pump site options due to its size and accessibility.
Pump site rotation follows similar principles to injection rotation but requires wider spacing. Previous sites need longer recovery periods due to extended cannula presence. Mark old sites with removable stickers to prevent premature reuse. Consider alternating between abdomen and alternative sites monthly.
Age-Specific Guidelines for Injection Sites
Children require modified approaches to places to inject insulin due to limited body surface area and fat tissue. The buttocks often provide the best injection site for young children, offering adequate fat tissue and reduced visibility. Parents should assist with injections until children develop sufficient motor skills and understanding.
Adolescents face unique challenges with injection site management during growth spurts and puberty. Rapid body changes alter fat distribution and insulin sensitivity. Increased self-consciousness may lead to site overuse in less visible areas. Education about proper rotation becomes crucial during this developmental stage.
Elderly Considerations
Older adults may have reduced subcutaneous fat and skin elasticity affecting suitable places to inject insulin. Arthritis or vision problems complicate self-injection and site rotation. Simplified rotation schemes using fewer sites may improve adherence while maintaining tissue health.
Cognitive changes in elderly patients necessitate injection site monitoring by caregivers. Clear marking systems using colored stickers or charts help maintain rotation schedules. Regular skin assessments detect problems before they affect blood sugar control.
Pregnancy Injection Modifications
Pregnancy dramatically alters abdominal injection site availability as the baby grows. Early pregnancy allows normal abdominal use, but expanding uterus gradually reduces accessible area. Lateral abdomen areas remain usable longer than central regions. Third trimester often requires complete transition to alternative sites.
Thigh and arm sites become primary places to inject insulin during late pregnancy. Increased blood flow during pregnancy may accelerate absorption from all sites. Frequent blood sugar monitoring helps identify necessary dose adjustments as injection sites change.
Advanced Injection Techniques and Tips
Skin preparation affects injection comfort and infection risk at all places to inject insulin. Clean sites with soap and water or alcohol swabs if visibly dirty. Allow alcohol to dry completely before injection to prevent stinging. Routine alcohol use for clean skin is unnecessary and may cause dryness.
Proper needle insertion technique ensures consistent subcutaneous delivery. Insert needles quickly and smoothly at the appropriate angle for your body type. Inject insulin slowly and steadily, counting to ten before withdrawal. This deliberate pace prevents insulin leakage and ensures complete dose delivery.
Temperature and Timing Strategies
Strategic use of temperature can optimize absorption from different places to inject insulin based on needs. Gentle site warming before rapid-acting insulin injection accelerates meal coverage. Avoiding heat exposure after long-acting insulin injection maintains steady basal delivery.
Timing injection site selection around daily activities maximizes absorption predictability. Morning abdominal injections provide consistent absorption for breakfast coverage. Evening thigh injections offer slower absorption suitable for overnight basal insulin. Weekend injection patterns might differ from weekday routines based on activity changes.
Troubleshooting Absorption Issues
Inconsistent blood sugar control despite proper dosing often indicates injection site problems. Systematically evaluate all places to inject insulin for signs of lipodystrophy or overuse. Temporary use of fresh sites helps determine if locations cause absorption issues.
Document absorption patterns from different sites through careful blood sugar monitoring. Note injection location, dose, timing, and subsequent glucose readings. Patterns emerging over several weeks guide site selection optimization. Share these records with healthcare providers for professional analysis.
Looking for cost-effective GLP-1 medications? Buy cheap Ozempic from a Canadian pharmacy partner through Better You Rx and enjoy significant savings on your diabetes prescriptions.
Safety Measures and Best Practices
Preventing infection at places to inject insulin requires basic hygiene practices. Wash hands before handling insulin and injection supplies. Never share needles or insulin pens between individuals. Replace needle tips after each use to maintain sterility and sharpness.
Proper insulin storage preserves medication effectiveness and injection safety. Refrigerate unopened insulin but never freeze. Room temperature storage for opened insulin prevents injection discomfort. Discard insulin exposed to extreme temperatures or past expiration dates.
Emergency Preparedness
Maintain accessible injection sites even during illness or injury. Identify backup places to inject insulin in case primary sites become unavailable. Practice non-dominant hand injection techniques for situations limiting mobility. Keep injection supplies in multiple locations for emergency access.
Travel preparation includes planning injection site rotation across time zones and climates. Pack extra supplies accounting for potential site problems or absorption changes. Research medical facilities at destinations for emergency support. Carry documentation of insulin requirements and injection needs.
Technology Integration
Modern technology assists with managing places to inject insulin effectively. Smartphone apps track rotation schedules and send reminders. Continuous glucose monitors reveal absorption patterns from different sites. Smart insulin pens record injection locations and doses automatically.
Digital photography documents injection site conditions over time. Weekly photos under consistent lighting show subtle changes. Cloud storage creates accessible records for healthcare provider review. Time-lapse comparisons reveal gradual tissue changes requiring intervention.
Final Recommendations
Successfully managing places to inject insulin requires systematic planning and consistent execution. Proper site rotation prevents tissue damage while maintaining predictable absorption. Regular site assessment identifies problems before they affect blood sugar control. Individual factors like body composition and activity levels guide personalized injection strategies.
Education about injection techniques and site management empowers better diabetes control. Understanding how different factors affect absorption enables informed decision-making. Recognizing early signs of site problems prevents complications. Continuous learning about new techniques and technologies improves outcomes.
Healthcare provider partnership optimizes injection site management over time. Regular reviews ensure rotation strategies remain appropriate as needs change. Professional assessment identifies subtle problems requiring intervention. Collaborative approaches address challenges while maintaining blood sugar targets.
Long-term success depends on establishing sustainable injection routines. Simple rotation systems promote adherence better than complex schemes. Flexibility accommodates lifestyle changes without compromising site health. Patience during adjustment periods allows new patterns to become habitual.
Frequently Asked Questions
How do I know if I’m injecting insulin correctly?
Correct injection technique produces minimal discomfort and consistent blood sugar results. The needle should enter smoothly without resistance, and insulin should flow easily without leakage. After injection, little to no insulin should appear on the skin surface. Blood sugar readings should respond predictably to doses when using proper technique at appropriate places to inject insulin.
What happens if you inject insulin in the wrong place?
Injecting into muscle instead of fat tissue causes rapid, unpredictable absorption potentially leading to hypoglycemia. Overused sites with lipodystrophy absorb insulin erratically, causing blood sugar swings. Injection into scar tissue or bruised areas may prevent proper absorption entirely. Wrong site selection can result in poor diabetes control despite correct dosing.
Should I pinch my skin when injecting insulin?
Skin pinching depends on needle length and body composition at chosen places to inject insulin. Short 4-6mm needles rarely require pinching for adults with adequate subcutaneous fat. Longer needles or lean body areas benefit from gentle pinching to ensure subcutaneous delivery. Pinch skin gently between thumb and fingers without squeezing tightly.
What are the two common insulin errors?
The most common insulin errors involve incorrect site rotation leading to lipodystrophy and failing to rotate among different places to inject insulin. Second, improper injection timing relative to meals causes blood sugar mismatches. These errors compound each other, as lipodystrophy makes timing effects more unpredictable.
What is the best location to inject insulin?
The abdomen generally provides the best combination of accessibility, absorption consistency, and rotation capacity. However, the optimal location varies by individual factors and insulin type. Rapid-acting insulin works best in the abdomen, while long-acting performs well in any appropriate site with adequate fat tissue.
How to use insulin injection during pregnancy?
During pregnancy, gradually transition from abdominal to alternative places to inject insulin as the belly expands. Use lateral abdomen areas as long as comfortable, then move to thighs and arms. Increase rotation frequency to accommodate reduced available sites. Monitor absorption changes due to increased blood flow and adjust doses accordingly.
Is it ok to inject insulin in my thigh?
Thigh injections work well for insulin delivery, particularly for long-acting formulations. Use the outer thigh area maintaining distance from knee and groin. Avoid injection before leg exercise which accelerates absorption. Thighs offer excellent rotation capacity for people requiring multiple daily injections across various places to inject insulin.