Managing diabetes means keeping your insulin in perfect condition, and proper storage is absolutely critical for maintaining its effectiveness. If you’ve ever wondered “does insulin need to be refrigerated,” you’re asking the right question. The answer affects not just your medication’s potency, but your overall health and blood sugar control.
Insulin is a delicate protein that can lose its effectiveness when exposed to extreme temperatures, light, or improper storage conditions. Getting the storage basics right means your medication works as intended, your blood sugar stays stable, and you avoid potentially dangerous complications from degraded insulin.
In this guide, we’ll walk you through everything you need to know about insulin storage, from refrigeration requirements to travel tips, so you can keep your medication safe and effective.
Need reliable insulin supplies? Browse our insulin collection for trusted diabetes management options.
Understanding Insulin and Storage Requirements
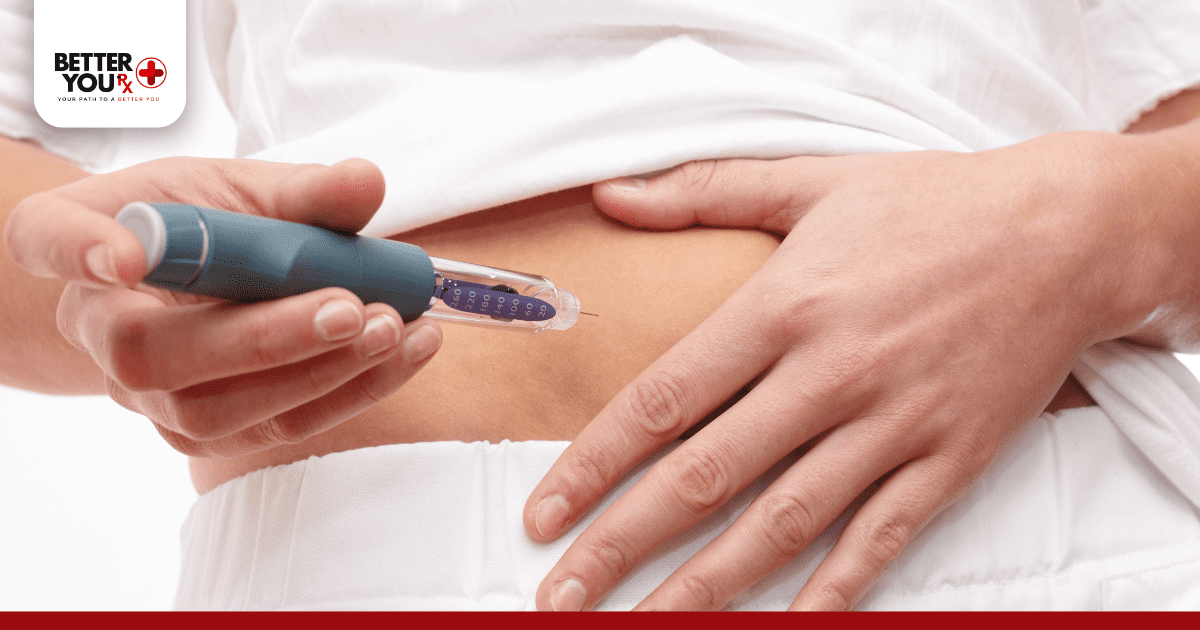
Insulin is a hormone that helps your body regulate blood sugar levels. When you have diabetes, your body either doesn’t produce enough insulin or can’t use it effectively. That’s where insulin medications come in, providing the hormone your body needs to function properly.
The challenge with insulin is that it’s a protein-based medication, which makes it sensitive to temperature changes, light exposure, and physical stress. Unlike some medications that remain stable at room temperature, insulin requires specific storage conditions to maintain its potency.
Why Temperature Matters for Insulin
Temperature control is the most important factor in insulin storage. Here’s what happens when insulin is exposed to different temperature ranges:
- Too Cold (Freezing): Insulin that freezes becomes completely unusable and must be discarded. The protein structure breaks down permanently, making the medication ineffective.
- Too Hot: High temperatures cause insulin to degrade rapidly, reducing its effectiveness and potentially making it dangerous to use.
- Proper Range: Most insulin types remain stable when stored between 36°F to 46°F (2°C to 8°C) in unopened vials or pens.
Understanding these temperature requirements helps you make informed decisions about where and how to store your insulin supplies.
Different Types of Insulin Storage Needs
Not all insulin types have identical storage requirements, though most follow similar guidelines. Here’s how different insulin categories should be handled:
| Insulin Type | Unopened Storage | After Opening | Room Temperature Duration |
| Rapid-acting | Refrigerate 36-46°F | Can stay at room temp | 28 days |
| Short-acting | Refrigerate 36-46°F | Can stay at room temp | 28-42 days |
| Intermediate-acting | Refrigerate 36-46°F | Can stay at room temp | 42 days |
| Long-acting | Refrigerate 36-46°F | Can stay at room temp | 28-42 days |
| Pre-mixed | Refrigerate 36-46°F | Can stay at room temp | 10-28 days |
These timeframes can vary between manufacturers, so always check your specific insulin’s packaging or insert for precise storage instructions.
Looking for specific insulin options? Check out our Basaglar Cartridge for long-acting insulin needs.
Does Insulin Need to Be Refrigerated: The Complete Answer
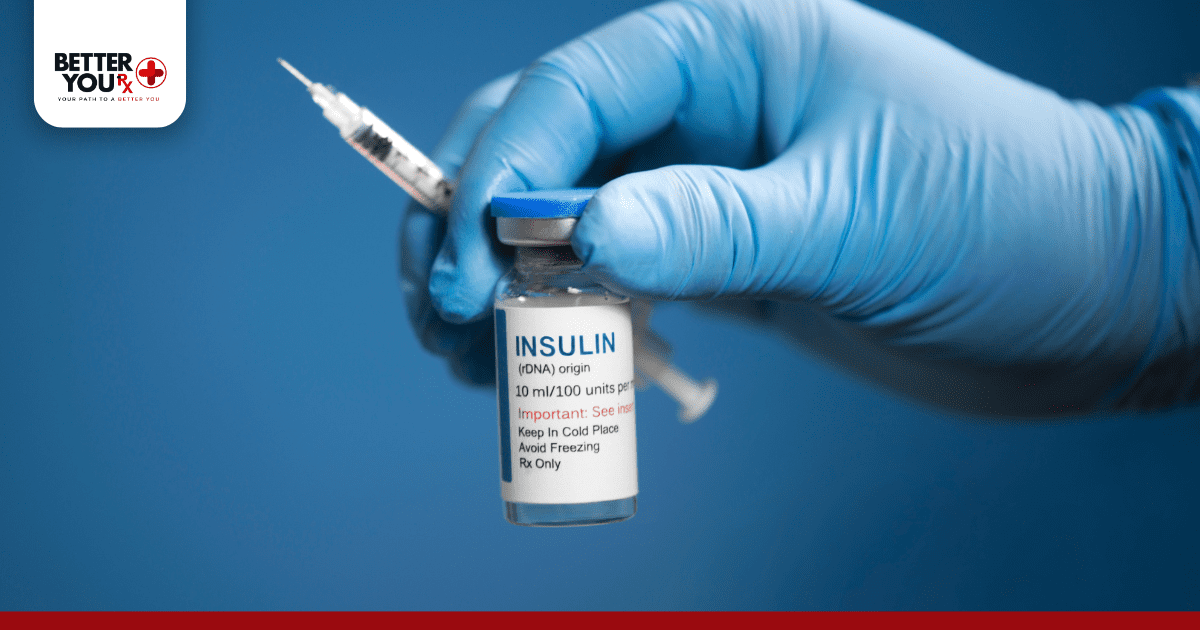
The short answer is: yes, unopened insulin should be refrigerated, but opened insulin can be stored at room temperature for limited periods. However, the complete picture is more nuanced and depends on several factors.
Unopened Insulin Storage
Unopened insulin vials, pens, and cartridges must be stored in the refrigerator between 36°F to 46°F (2°C to 8°C). This keeps the medication stable until its expiration date. Key points for unopened insulin storage:
- Store in the main body of the refrigerator, not the door where temperatures fluctuate
- Keep insulin in its original packaging to protect from light
- Never store insulin in the freezer compartment
- Don’t store near the back wall where temperatures might be coldest
- Maintain consistent temperature by avoiding frequent door opening
Opened Insulin Storage Options
Once you start using an insulin vial or pen, you have two storage options:
Option 1: Continue Refrigerating
- Keeps insulin stable for longer periods
- Must warm to room temperature before injecting
- Good for people who use insulin infrequently
Option 2: Room Temperature Storage
- More convenient for daily use
- No need to warm before injection
- Must be used within specific timeframes (usually 28-42 days)
- Store between 59°F to 86°F (15°C to 30°C)
Most diabetes educators recommend room temperature storage for daily-use insulin because it’s more comfortable for injections and reduces the risk of lipodystrophy (changes in fat tissue under the skin).
Special Considerations for Different Situations
Your insulin storage approach might need adjustments based on your lifestyle and circumstances:
- Frequent Travelers: Consider keeping unopened backup supplies refrigerated while using opened insulin at room temperature
- Hot Climates: Room temperature storage becomes riskier in extremely hot weather
- Irregular Use: If you don’t use insulin daily, refrigerated storage might be better for opened supplies
Need diabetes management support? Explore our Byetta for additional blood sugar control options.
Best Practices for Insulin Storage
Proper insulin storage goes beyond just temperature control. Following these best practices ensures your medication stays effective and safe to use.
Refrigeration Guidelines
When storing insulin in the refrigerator, location and method matter:
Optimal Refrigerator Placement:
- Store in the main compartment, never the door
- Use the crisper drawer or a dedicated medication area
- Keep insulin toward the front where temperatures are most stable
- Avoid areas near the cooling vents or back wall
Organization Tips:
- Use a small container or organizer to keep insulin supplies together
- Label opened insulin with the date you first used it
- Rotate stock by placing newer supplies behind older ones
- Keep a thermometer in your medication storage area
Room Temperature Storage Best Practices
For insulin stored at room temperature, consistency and protection are key:
- Choose a cool, dark place away from direct sunlight
- Avoid areas with temperature fluctuations like bathrooms or kitchens
- Never leave insulin in cars, especially during hot weather
- Use a medication organizer or small cooler for travel
- Keep insulin in its original packaging when possible
Protecting Insulin from Light and Physical Damage
Beyond temperature, insulin needs protection from other environmental factors:
Light Protection:
- Store in original cartons or opaque containers
- Avoid transparent pill organizers for insulin
- Keep away from direct sunlight and bright artificial lights
Physical Protection:
- Handle vials and pens gently to avoid damage
- Don’t shake insulin vigorously (gently roll if mixing is needed)
- Inspect for cracks or damage before each use
- Replace damaged supplies immediately
For fast-acting options, consider our Fiasp Vial for reliable rapid insulin delivery.
Signs Your Insulin May Be Compromised
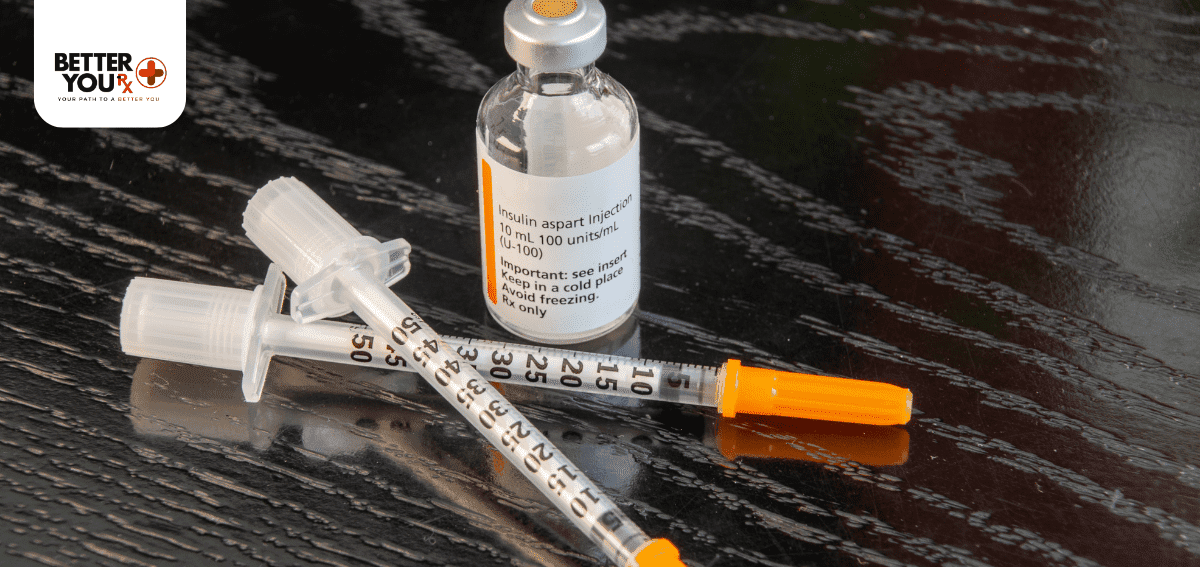
Recognizing when insulin has been compromised is crucial for maintaining effective diabetes management. Here are the key warning signs to watch for:
Visual Inspection Signs
Regular visual checks help you identify insulin that may no longer be effective:
Clear Insulin (Rapid and Long-Acting Types):
- Should remain completely clear and colorless
- Any cloudiness, particles, or discoloration means discard immediately
- Clumping or crystallization indicates the insulin is no longer safe to use
Cloudy Insulin (Intermediate-Acting and Some Mixed Types):
- Should have a uniform, milky appearance when properly mixed
- Clumping that doesn’t dissolve with gentle rolling indicates spoilage
- Unusual color changes or crystal formation means replacement is needed
Physical and Performance Indicators
Beyond visual cues, pay attention to how your insulin behaves and performs:
Physical Changes:
- Unusual thickness or consistency changes
- Separation that doesn’t remix with gentle agitation
- Frosted appearance (indicates previous freezing)
- Cracks or damage to vials or pen cartridges
Performance Issues:
- Blood sugar levels remaining consistently higher than expected
- Insulin not working as effectively as usual
- Unusual injection site reactions or irritation
- Burning or stinging sensation during injection
Temperature Exposure Warning Signs
Insulin exposed to extreme temperatures shows specific signs of damage:
- Insulin that has been frozen will often appear cloudy or have visible particles
- Heat-exposed insulin might change color or develop an unusual odor
- Insulin left in hot cars may appear normal but lose effectiveness
- Any insulin with an unusual smell should be discarded immediately
If you notice any of these signs, don’t risk using potentially compromised insulin. Replace it immediately and contact your healthcare provider if you have concerns about blood sugar control.
Travel and Emergency Storage Tips
Traveling with insulin or managing emergency situations requires special planning to ensure your medication stays safe and effective.
Air Travel Guidelines
Flying with insulin involves specific considerations for both carry-on and checked luggage:
Carry-On Recommendations:
- Always pack insulin in carry-on luggage, never checked bags
- Bring prescription labels and a letter from your doctor
- Pack extra supplies in case of delays or lost luggage
- Use insulated travel cases designed for medications
- Allow extra time for security screening procedures
TSA and International Guidelines:
- Insulin is allowed through security checkpoints without quantity restrictions
- Carry original prescription bottles or pen packaging
- Declare insulin and diabetes supplies during security screening
- Research destination country regulations for medication imports
Hot Weather Storage Solutions
High temperatures pose serious risks to insulin effectiveness, especially during summer travel or in warm climates:
Cooling Options:
- Invest in a medical-grade insulin cooling case
- Use cooling packs designed for medications (avoid direct ice contact)
- Consider battery-powered medication refrigerators for extended trips
- Plan for air conditioning failures or power outages
Heat Protection Strategies:
- Never leave insulin in parked vehicles
- Carry insulin in an insulated bag during outdoor activities
- Monitor local weather forecasts and plan accordingly
- Have backup cooling plans for emergencies
Emergency Preparedness
Natural disasters, power outages, and other emergencies require advance planning:
Emergency Kit Essentials:
- At least 7 days’ worth of insulin and supplies
- Battery-powered or manual cooling options
- Non-perishable snacks and glucose tablets
- Emergency contact information for healthcare providers
- Copy of prescriptions and medication lists
Power Outage Planning:
- Identify local pharmacies with backup power
- Know locations of cooling centers or facilities with refrigeration
- Have manual cooling options like cool wet towels
- Understand how long your refrigerator stays cold without power (typically 4-6 hours)
Proper preparation ensures you can maintain diabetes management even during unexpected situations or travel disruptions.
Summary: Key Takeaways for Insulin Storage
Proper insulin storage isn’t just about following rules, it’s about ensuring your diabetes management remains effective and your health stays protected. The question “does insulin need to be refrigerated” has a clear answer: yes for unopened supplies, with flexible options for opened insulin based on your usage patterns and lifestyle.
Temperature control remains the most critical factor in insulin storage. Whether you choose refrigerated or room temperature storage for opened insulin, consistency and protection from extreme temperatures, light, and physical damage are essential. Regular visual inspections and awareness of performance changes help you identify when insulin may be compromised.
Remember that different insulin types have varying storage requirements and timeframes. Always check your specific medication’s packaging for precise guidelines, and don’t hesitate to replace insulin that shows any signs of deterioration. Your health depends on using medication that maintains its full effectiveness.
For reliable insulin supplies and diabetes management support, explore our comprehensive medication options and consult with healthcare professionals about the best storage practices for your specific situation.
Frequently Asked Questions About Insulin Storage
How to know if insulin is spoiled?
Spoiled insulin shows several warning signs including cloudiness in normally clear insulin, clumping or crystallization, unusual color changes, or an odd smell. If your blood sugar levels remain consistently high despite normal insulin doses, this may also indicate compromised medication. When in doubt, replace the insulin and consult your healthcare provider.
Can you put insulin back in the fridge?
Once insulin has been stored at room temperature, it’s generally not recommended to return it to the refrigerator. The temperature fluctuation can affect the medication’s stability. However, if insulin was briefly exposed to room temperature (less than a few hours) and you prefer refrigerated storage, it’s typically safe to return it to the fridge. Always check with your pharmacist for specific guidance.
How can you tell if insulin is still good?
Good insulin should be clear and colorless (for rapid and long-acting types) or uniformly cloudy (for intermediate-acting types) with no clumping, particles, or unusual odors. It should maintain its normal consistency and continue to effectively control your blood sugar levels. Check the expiration date and note how long it’s been since opening, as effectiveness decreases over time even with proper storage.
How long does it take for insulin to go bad?
Unopened insulin remains effective until its expiration date when properly refrigerated. Once opened, most insulin types stay potent for 28-42 days at room temperature or longer if kept refrigerated. However, insulin exposed to extreme heat can degrade within hours, while frozen insulin becomes immediately unusable. The exact timeframe varies by insulin type and storage conditions.
What are the symptoms of bad insulin?
Using degraded insulin typically results in poor blood sugar control, with levels remaining higher than expected despite normal dosing. You might experience increased thirst, frequent urination, fatigue, or other hyperglycemia symptoms. Some people also report unusual burning or stinging at injection sites when using compromised insulin.
What happens if you take insulin that’s gone bad?
Using spoiled insulin can lead to dangerously high blood sugar levels since the medication won’t work effectively. This can result in diabetic ketoacidosis (DKA) or other serious complications if not addressed quickly. If you suspect you’ve used compromised insulin and experience symptoms like nausea, vomiting, or very high blood glucose readings, seek immediate medical attention and replace your insulin supply.



